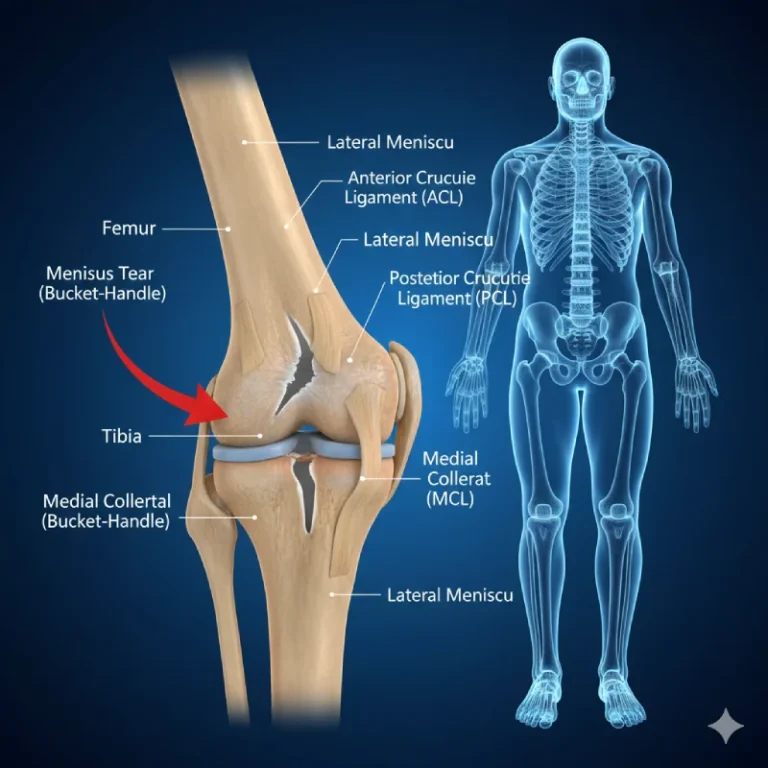
Back pain, especially when radiating to the legs (sciatica), can become an insurmountable obstacle to daily activities
Epidural steroid injections (ESI), commonly known as a “back blockade,” are often presented as a “quick fix.” However, from a clinical research perspective, the picture is much more nuanced. In this article, we analyze whether this procedure truly “cures” or merely masks symptoms, and what leading global medical institutions say about it.
What exactly is an epidural blockade?
An epidural blockade is not a simple pain-relieving shot. It is a precise medical procedure during which a mixture of corticosteroids (anti-inflammatory agents) and local anesthesia is injected into the epidural space—the area surrounding the spinal cord lining.
Anatomical context
Our spinal canal houses nerve roots. When an intervertebral disc herniates or the canal narrows (stenosis), the nerve becomes mechanically irritated. This irritation triggers a chemical inflammatory cascade. A back blockade targets this inflammation specifically, rather than the mechanical obstruction itself.
Does a back blockade really work?
International studies, including Cochrane database analyses, point to a significant fact: the effectiveness of epidural blockades is highest in the short term.
- Short-term relief (2–6 weeks): Approximately 70–80% of patients report significant pain reduction.
- Long-term perspective (6+ months): Research shows that after one year, outcomes between those who received a blockade and those who only underwent physiotherapy often equalize.
Conclusion: A blockade is not a cure in the literal sense. It is a “strategic pause” in pain, allowing the patient to begin aggressive physiotherapy that was previously impossible due to the intensity of the pain.
When is a back blockade justified?
Based on North American Spine Society (NASS) guidelines, a blockade is indicated in the following cases:
- Lumbar radiculopathy – pain, tingling, or weakness radiating along a nerve (usually from a disc herniation).
- Spinal stenosis – narrowing of the canal that causes pain while walking.
- Spondylolisthesis – displacement of a vertebra that irritates nerve roots.
Important: If pain is localized only in the lower back without radiation to the legs, the effectiveness of an epidural blockade is significantly lower. In such cases, the problem often lies in the facet joints, not the epidural space.
The process of a back blockade
There are three main methods:
- Transforaminal blockade – the most effective and specific. Medication is injected directly into the opening where the nerve exits the spine.
- Interlaminar blockade – a more traditional approach where the needle is inserted between two vertebrae.
- Caudal blockade – an injection through the sacral canal, often used in more complex cases or following surgeries.
Procedure steps
- Positioning – the patient sits on a couch, placing their hands on their knees.
- Local anesthesia – the skin is numbed with a local anesthetic.
- Insertion of the epidural needle – the doctor guides the needle directly into the epidural space.
- Administration of medication – the steroid and anesthetic mixture is injected.
Risks
While the procedure is relatively safe, it is invasive. International data indicates the following risks:
- Dural puncture – can cause severe headaches lasting for days.
- Infection risk – rare, but an epidural abscess can be life-threatening.
- Steroid side effects – temporary increase in blood pressure and blood sugar levels (critical for diabetics), and sleep disturbances.
- Nerve damage – extremely rare if the procedure is performed by an experienced specialist under fluoroscopic control.
An epidural blockade for the back is a powerful tool in the fight against radicular pain, but it is not a miracle cure. It is most effective as part of a multimodal treatment plan.
The gold standard: If pain does not subside after 6 weeks of conservative treatment and interferes with quality of life, a blockade may be the next step before surgical intervention. However, if the blockade does not improve the condition after a second attempt, continuing this therapy usually yields no benefit.

Dr. Jānis Margevičus
FAQ
Typically, the local anesthetic begins to work immediately (within the first few hours), providing initial relief. However, the full anti-inflammatory effect of the steroids usually becomes apparent within 2 to 7 days.
The internationally accepted standard is no more than 3 to 4 times per year. Excessive use of corticosteroids can lead to the weakening of local tissues, such as ligaments and vertebrae.
In cases of chronic pain involving scar tissue (fibrosis) or central sensitization, the effectiveness of the injection is significantly lower than during the acute inflammatory phase. A consultation with a specialist is necessary to determine if this is the right approach for long-standing issues.
The price for an epidural blockade at our clinic in the center of Riga is €120.00.