In this article, we will look at the possible causes of iron deficiency, as well as diagnostic and treatment options provided by family doctors and gynecologists. We will clarify what iron deficiency in the body is, why it occurs, and where to seek help for this problem.
What is the iron-deficiency anemia?
Iron deficiency anemia is the most common nutritional deficiency anemia in the world. Its causes are simple: insufficient iron intake through diet, poor absorption, increased requirements (most commonly during pregnancy), and blood loss (menstruation, gastrointestinal bleeding). Global reviews and clinical guidelines consistently emphasize that iron deficiency anemia is common and treatable, but its cause must always be purposefully investigated.
The World Health Organization indicates that hundreds of millions of women and children live with anemia; iron deficiency is the most common cause. It is not just “fatigue”—anemia directly affects mortality, maternal and child outcomes, and quality of life.
The role of iron in the body and the importance of “heme iron”
Iron is a component of hemoglobin and myoglobin, participating in electron transfer and hormone synthesis. In the diet, iron exists in two forms: heme iron (animal products) and non-heme iron (plant products). It is believed that heme iron is absorbed better. A typical “Western” diet provides approximately 10–15% of total iron intake, yet this proportion contributes disproportionately to absorption.
To ensure normal iron levels in the blood, it is necessary to combine non-heme iron (legumes, green leafy vegetables) with Vitamin C and/or a small amount of heme iron sources (meat, fish) to improve absorption.
Iron deficiency symptoms: when to think about blood tests?
Most often, patients complain of fatigue, weakness, shortness of breath during exertion, paleness, dizziness, headaches, and palpitations. Cracking at the corners of the mouth, brittle nails, and hair loss are also signs of iron deficiency. These symptoms are non-specific, so diagnosis is based on blood tests.
In rarer cases, patients develop a desire to eat unusual things, such as chalk or ice—PICA syndrome. PICA is not a “whim” but is often associated with changes in the brain’s dopamine system and taste perception affected by iron deficiency in the body.
Iron deficiency calculation
Iron deficiency calculator
(Includes 500 mg for iron store replenishment)
What does "low iron" mean and what tests are required?
Daily, patients often want to find out their "blood iron level," but a standalone serum iron measurement is variable and insufficient for diagnosis. To determine a decreased iron level in the blood, international guidelines recommend performing expanded blood tests:
- Full blood count – determines erythrocyte count, hemoglobin, hematocrit, and erythrocyte indices (MCV, MCH, MCHC) to classify the anemia.
- Ferritin – the primary marker of tissue iron stores.
- Transferrin saturation (TSAT) – shows the availability of circulating iron.
- CRP (C-reactive protein) – must be determined if inflammation is suspected, as inflammation raises ferritin regardless of iron status.
- Soluble transferrin receptor (sTfR) – useful because inflammation can mask iron deficiency.
Diagnostic thresholds:
- Some medical associations suggest a ferritin threshold of 45 ng/mL rather than 15 ng/mL to avoid missing iron deficiency.
- In cases of chronic inflammation or chronic kidney disease, ferritin may be "misleadingly normal"; TSAT and other markers must also be evaluated.
- Normal blood iron levels for men are 80–180 µg/dL, and for women 60–160 µg/dL.
- A sufficient increase in hemoglobin (≥10 g/L) within 2 weeks of starting therapy practically confirms absolute iron deficiency—even if initial indicators were contradictory.
What drains iron from your body?
Iron deficiency is not the "end" of a diagnosis, but a signal to find the cause:
- Pre-menopausal women – the most common cause is menstrual bleeding; however, gastroenterology associations recommend considering gastroscopy and colonoscopy, as gastrointestinal pathologies can be asymptomatic.
- Men and women over 40 – gastroscopy and colonoscopy are recommended.
- If the cause of bleeding is not identified during endoscopy, a Helicobacter pylori biopsy is performed and treated if positive; for celiac disease, serology is performed with a biopsy only if the test is positive. Most often, Helicobacter pylori biopsies are performed as part of screening to ensure the absence of the
- bacteria in the gastric mucosa.
If iron deficiency is suspected and symptoms are observed, we recommend visiting a family doctor, who coordinates initial tests and starts oral iron supplements, evaluates the risk of bleeding or gastrointestinal absorption disorders, and refers to a gastroenterologist for endoscopy or a gynecologist in cases of heavy menstruation or uterine fibroids.

Dr. Viktorija Margevičus

Dr. Ruslans Mihailovskis

Dr. Denis Jevdokimov
Iron deficiency anemia and pregnancy
During pregnancy, iron requirements increase rapidly as maternal blood volume expands by ~40–50%, requiring more iron for fetal and placental development. Iron deficiency is linked to premature birth, low birth weight, placental and postpartum complications, and impacts on fetal brain development. Iron deficiency and iron deficiency anemia during pregnancy are common but often go unrecognized and untreated.
The American College of Obstetricians and Gynecologists recommends blood test screening with a full blood count in the 1st trimester and at 24–28 weeks. If anemia is confirmed, blood iron levels must be evaluated and treatment—intravenous or oral iron supplements—must be initiated.
Elevated blood iron – when does it become a problem?
While this article focuses on deficiency, we observe in clinical practice that patients may have elevated blood iron levels (e.g., after IV iron, chronic transfusions, or rare metabolic disorders). When interpreting isolated "serum iron," its high variability must be remembered. Clinical significance lies in ferritin levels, transferrin saturation, and the clinical context (inflammation, liver disease, hemochromatosis). Evaluation of these indicators should be performed by a family doctor.
Iron deficiency anemia treatment
Diet and lifestyle
- Include heme iron (beef, liver, seafood) and non-heme iron (legumes, spinach, whole grains).
- Combine with Vitamin C and avoid drinking tea/coffee directly during meals, as tannins inhibit absorption.
Oral iron supplements
- Guidelines recommend starting with oral iron unless there is intolerance or absorption issues.
- Studies on lower doses or less frequent use (e.g., every other day) show better tolerance and similar efficacy because hepcidin regulation affects absorption; practically—adjust the dose to reach Hb +10 g/L in 2–4 weeks.
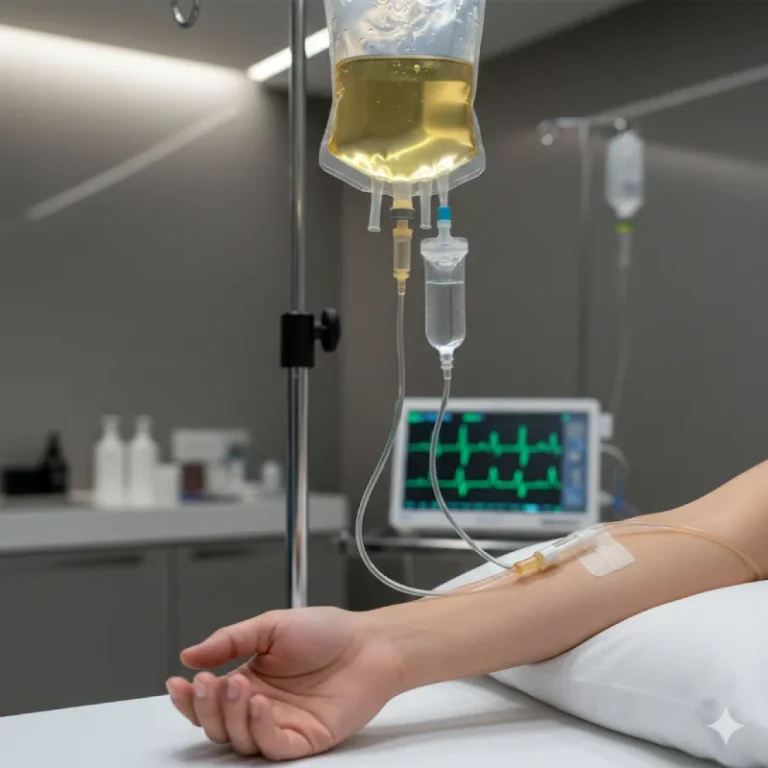
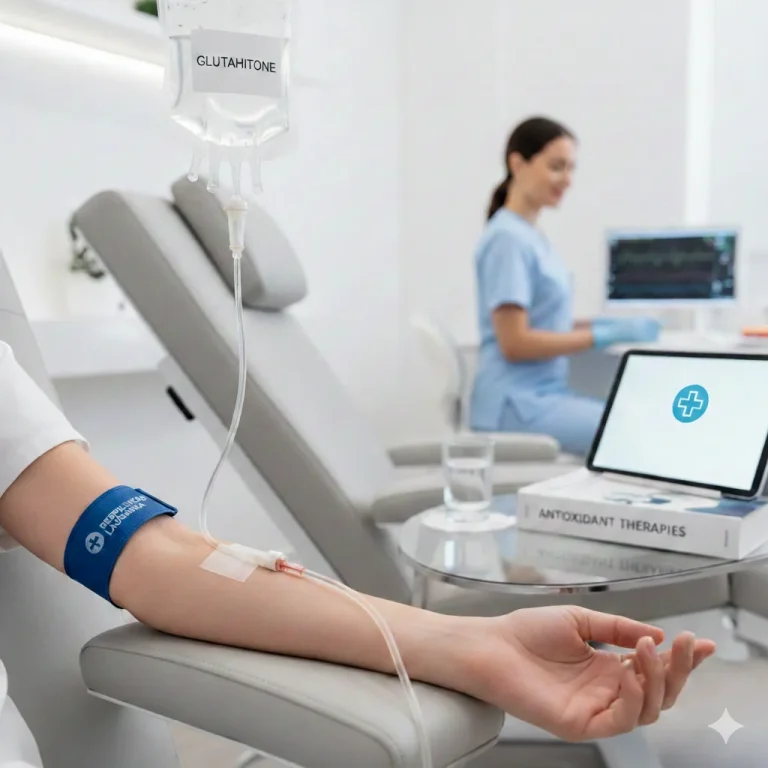
Intravenous iron infusions in Riga center - Venofer or Monofer infusions
Intravenous iron infusions are more effective and faster for improving Hb and ferritin in situations with poor tolerance/absorption or an urgent need for correction (e.g., before major surgery, or in the third trimester of pregnancy with severe anemia).
Monofer iron infusions
A modern, high-concentration preparation. Its structure allows for a very high dose of iron (even the full course) in a single infusion lasting approximately 15–30 minutes. The ampoule itself is more expensive, but you save time and money on repeat visits.
*Price is €185 for 5 Monofer ampoules.
Venofer iron infusions
A classic choice, but its molecular structure does not allow for a large dose at once. This means you will need to visit the day hospital several times (usually 2–5 visits).
Iron deficiency treatment - step by step
Diagnosis and cause seeking
The first step is more than just identifying a low number; it’s about uncovering the "why." A clinician will typically start with a deep dive into your medical history, focusing on dietary habits, menstrual patterns, or potential gastrointestinal issues. It is crucial to determine if the deficiency stems from inadequate intake, increased demand (such as intense athletic training or pregnancy), or chronic blood loss. Without addressing the underlying cause, any treatment serves only as a temporary fix, which is why diagnostic tests like ultrasounds or endoscopies are often ordered alongside blood work.
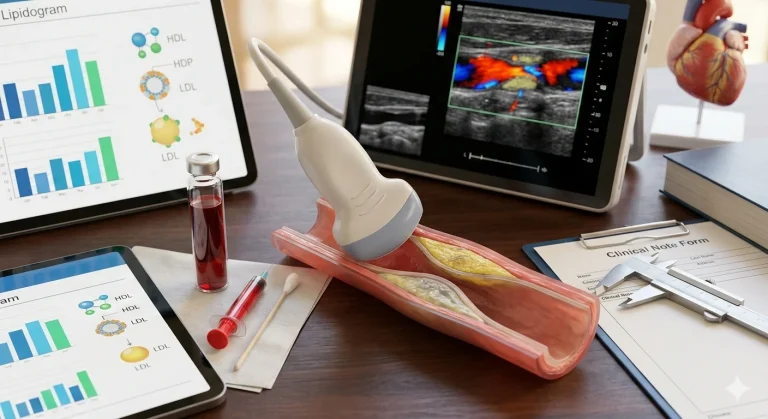
Lab Tests: FBC, Ferritin, and Transferrin saturation
To get a complete picture of your status, checking just your hemoglobin isn't enough. A full blood count (FBC) shows the number and size of your red blood cells, while ferritin is the gold standard for measuring your body’s "storage tanks." Because ferritin can falsely rise due to inflammation, doctors also check transferrin saturation, which indicates how much iron is actually available for transport to your tissues. This set of markers serves as your baseline to track real-time progress during therapy.
Oral iron supplements
If the iron deficiency is mild to moderate, the standard approach is oral supplementation (usually 40–65 mg of elemental iron). Modern protocols increasingly suggest every-other-day dosing, as this can improve absorption and significantly reduce common side effects like constipation or nausea. While you might start feeling a subtle lift in energy after a few weeks, the course typically lasts 6–8 weeks to ensure that you aren't just raising your hemoglobin, but also refilling your depleted long-term stores.
Intravenous iron infusions or "Iron IV therapy"
In some cases, oral pills are either ineffective or unsuitable, leading to the recommendation of an intravenous iron infusions. This method delivers iron directly into the bloodstream, bypassing the digestive system entirely. It is a faster, more potent route that requires medical supervision. This path is chosen under specific circumstances:
- Malabsorption and chronic conditions - for those with Celiac disease, IBS, or chronic kidney and heart failure, the body often cannot physically absorb iron through the gut due to inflammation or functional damage. In these cases, IV therapy is the only reliable way to ensure the iron reaches its destination.
- Intolerance or failure to reach goals - if a patient suffers from severe GI side effects (nausea, cramping) or if follow-up labs show that oral supplements failed to raise iron levels after two months, the "bypass" route via IV is used.
- Rapid correction needed - in situations where time is a luxury you don’t have—such as right before a major surgery to minimize transfusion risks, or during the 3rd trimester of pregnancy when both mother and baby require immediate stabilization.
Frequently Asked Questions
If your levels are dangerously low or you have an upcoming surgery/event, intravenous (IV) iron infusions is the only way to raise levels "instantly."
"Brick Wall" fatigue, "brain fog", PICA syndrome, restless leg syndrome and physical changes - noticeable hair thinning, brittle or "spoon-shaped" nails, and a smooth, sore, or unusually pale tongue.
Effective treatment follows a three-step clinical process to ensure you aren't just masking symptoms, but solving the root cause.
Step 1: Before starting any treatment, consult a family doctor or gynecologist. It is vital to identify the "source of the leak" (e.g., heavy periods or GI issues) through blood tests. A doctor will look beyond basic hemoglobin to check ferritin (stored iron) and transferrin saturation (circulating iron).
Step 2: For mild to moderate deficiency, doctors typically prescribe 40–65 mg of elemental iron. To speed up results, take these on an empty stomach with Vitamin C. Note that oral therapy is a marathon, often requiring 3–6 months to fully refill your body’s iron stores.
Step 3: If oral pills cause severe side effects, aren't being absorbed (due to IBS or Celiac), or if you need to raise levels rapidly (such as during the 3rd trimester of pregnancy or before surgery), IV Iron therapy is the most effective route. It bypasses the gut to deliver iron directly into the bloodstream, often correcting the deficiency in just one or two sessions.