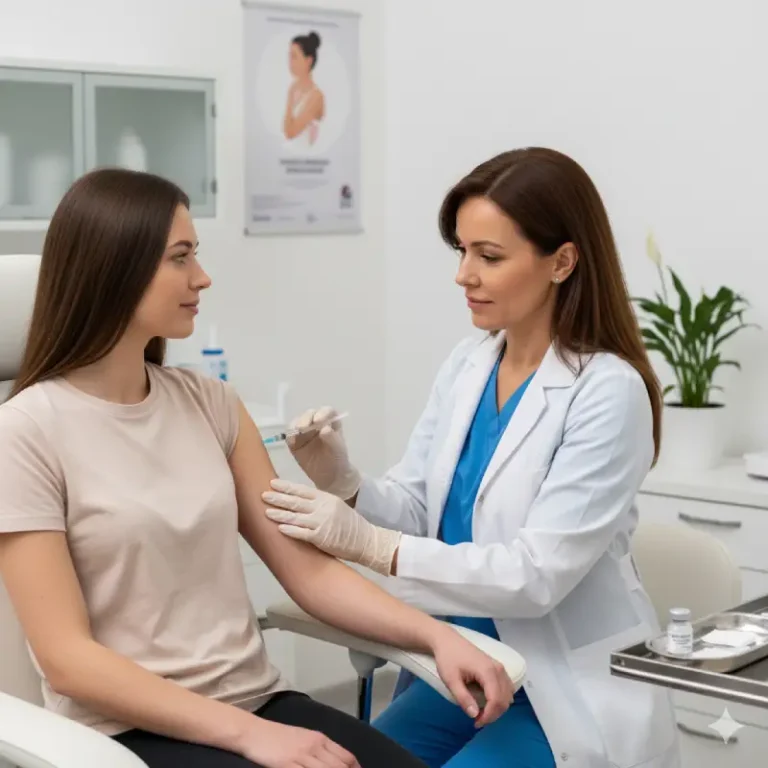
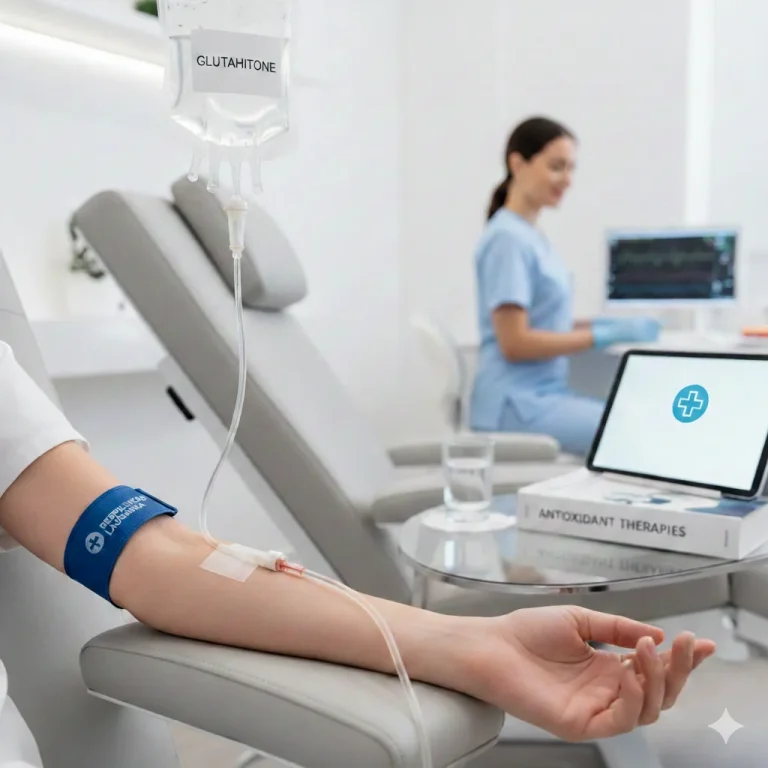
Intravenous (IV) therapy is one of the most essential medical methods used in emergency care, the treatment of chronic diseases, and for preventative purposes. It involves the administration of solutions and medications directly into the bloodstream, ensuring a rapid and effective impact. Unlike oral preparations, the medications used in infusion therapy bypass the digestive system and enter the body with maximum bioavailability.
This method allows for precise control of the administered dose, provides an immediate effect, and is indispensable in situations where urgent assistance is required or when a patient cannot take medications orally.
What is intravenous therapy?
Intravenous therapy refers to the administration of solutions and medications into a vein using a dropper or an infusion system. It can be short-term (e.g., during a single procedure) or long-term (e.g., in the treatment of oncology patients).
- Direct entry into the bloodstream ensures rapid action.
- The medication composition is selected individually based on the patient’s diagnosis, lab results, and general health status.
- The duration of the procedure can vary from 30 minutes to several hours, depending on the solution and medication being administered.
Before starting infusion therapy, a consultation with a General Practitioner (GP) and examinations are required:
- Blood tests (electrolytes, kidney and liver function markers, hemoglobin).
- Health assessment to determine the most suitable medications and dosages.
- Screening for contraindications (e.g., kidney failure, heart failure, allergies).

Dr. Ruslans Mihailovskis
Main groups of medications used in infusion therapy
Various medications belonging to several pharmacological groups are used in intravenous therapy. Each has its own purpose and indications.
Electrolyte solutions
- Sodium chloride (0.9% physiological saline) – Fluid replacement and treatment of dehydration.
- Ringer’s lactate solution – Restoring electrolyte balance, especially after trauma or surgery.
- Potassium-containing solutions – For the correction of hypokalemia.
Glucose solutions
These provide energy and are used in cases of hypoglycemia or as a base for administering other medications.
Pain relievers and anti-inflammatory drugs
- NSAIDs (e.g., Diclofenac, Ketorolac) – For the reduction of acute pain.
- Opioids (e.g., Morphine) – For strong pain control, especially in oncology and the postoperative period.
Antibiotics and antimicrobial agents
- Broad-spectrum antibiotics (e.g., Ceftriaxone, Piperacillin/Tazobactam) – For treating severe infections.
- Antiviral and antifungal agents – For specific types of infections.
Intravenous vitamins
- Vitamin C – For strengthening immunity and antioxidant protection.
- B-group vitamins – For nervous system and metabolic support.
- Magnesium, Calcium – To improve muscle and heart function.
- Iron preparations (Monofer, Venofer) – For correcting iron deficiency anemia.
- Glutathione – A powerful antioxidant.
Hormonal preparations
- Corticosteroids (e.g., Dexamethasone) – For treating severe allergic reactions, autoimmune diseases, and inflammatory processes.
Indications for intravenous therapy
Intravenous therapy is widely utilized, and its indications include:
- Treatment of acute conditions (shock, severe dehydration, sepsis).
- Therapy for chronic diseases (oncology, autoimmune diseases).
- Treatment of infections with intravenous antibiotics.
- Provision of pain control.
- Preventative administration of vitamins and minerals for patients with malabsorption syndromes or following surgery.
Advantages of infusion therapy:
- Rapid and effective impact.
- Precise dosage control.
- Ability to administer medications to patients who cannot take them orally.
- Wide range of applications – from emergency care to long-term therapy.
Possible risks and side effects
- Risk of infection if sterility is not maintained.
- Allergic reactions to medications.
- Electrolyte imbalance if dosages are not chosen correctly.
- Vein irritation and thrombophlebitis.
Therefore, infusion therapy should only be performed by medical personnel with appropriate training and in suitable conditions. Infusion therapy should not be trusted to be performed in a home setting.
The global importance of infusion therapy
Infusion therapy is an integral part of modern medicine. It is used in hospitals, outpatient clinics, and even home care. In developed countries, ports and central venous catheters are increasingly used, allowing for long-term medication administration for patients with chronic illnesses.
Future perspectives
Intravenous therapy continues to evolve and is becoming increasingly personalized. The latest research looks at possibilities for creating medication combinations based not only on blood tests but also on genetic tests and individual metabolic characteristics. This means that in the future, patients could be offered even more precisely tailored solutions.
It is predicted that infusion therapy will become even more accessible outside of hospitals—in specialized clinics and home care. Simultaneously, technologies are developing that allow for safer control of the administered dose and monitoring of the patient’s condition during the procedure.
Overall, infusion therapy will become an even more integrated part of healthcare—used not only for acute conditions but also for prevention, chronic disease control, and improving quality of life.
In IV therapy, vitamins enter the bloodstream directly, ensuring 100% absorption and immediate nutrient supply to the cells. This allows for much higher concentrations that cannot be achieved with tablets.
Yes, the procedure is safe if performed by medical personnel after a consultation with a doctor.
For acute situations (e.g., after recovering from a virus, heavy physical exertion, or a “hangover”), a single procedure is often sufficient to feel an immediate surge of energy. For treating chronic fatigue or deficiencies, doctors usually recommend a course (e.g., once a week for 4–6 weeks).